

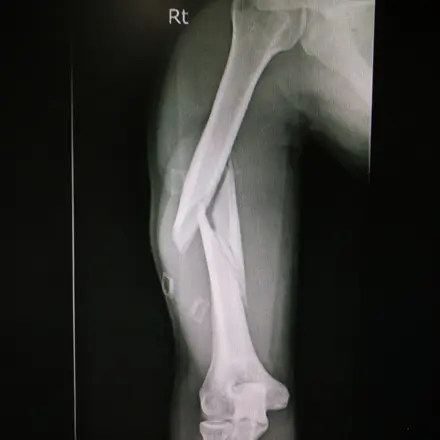
The patient was a 7 year old male who fell from a high bar at gymnastics sustaining a type 3 supracondylar humerus fracture on. He was treated with closed reduction and percutaneous pinning surgery by the pediatric orthopedic surgeon. He was seen in clinic for follow-up by the surgeon and had pins removed on approximately 30 days post-operatively. He developed cubitus varus hyperextension malunion of his elbow fracture.
Was there a breach in the standard of care that resulted in the cubitus varus hyperextension malunion? What errors occurred during and after the surgery that resulted in the malunion? Should the doctor have been able to diagnose the issue from the follow up visit?
An AMFS Pediatric Orthopedic Surgery expert reviewed this matter and opined that, to a reasonable degree of medical certainty, the surgeon violated the medical standard of care in the performance of the closed reduction and percutaneous pinning surgery. While the reduction was adequate, the pinning did not cross the fracture site and therefore could not stabilize the fracture. The fluoroscopy images taken on the date of surgery and the radiographs from one and two weeks subsequent to surgery demonstrate that the pins were placed above the fracture site. Thus, the pins did not engage the distal fragment, did not cross the fracture site, and did not stabilize the fracture. The inadequate pinning of the fracture allowed the fracture to displace to a varus and hyperextension position. The patient has a complication of cubitus varus and extension malunion. There is substantial deformity noted on both radiographs and on the clinical photos. On physical examination by another surgeon, he was noted to have obvious deformity, hyperextension, and lack of flexion. This deformity is unlikely to remodel. He will have cosmetic deformity. He will have functional limitations with hyperextension and lack of flexion. He will have difficulty with weight bearing sports such as gymnastics. He is at increased risk for lateral condyle fracture. He will likely require corrective surgery which would involve distal humerus osteotomy. This is a complex upper extremity deformity corrective surgery that has risks of neurovascular injury, non-union, malunion, and stiffness.
The medical expert witness partner for attorneys serious about building a winning case
AMFS is your trusted source for highly-qualified medical expert witnesses. After pioneering the field nearly three decades ago, we’re continuing to redefine medical expert witness services by providing value far beyond a referral alone.
Our Physician Medical Directors know what it takes to build a strong case. Our medical expert witnesses leave no doubt. And our case managers streamline billing and logistics every step of the way, letting you focus on what you do best: constructing your winning case. Explore why AMFS clients expect more from their medical expert witnesses—and get it.
